Osteoporosis is not just an “old woman’s disease.” Although it is more common in white or Asian women over the age of 50, osteoporosis can occur in almost any person, women and men, at any age. In women, bone loss can begin as early as age 25 years. 45% of fractures in women aged 50 and over are due to underlying osteoporosis (3). In fact, about 75 million people are currently affected by osteoporosis in the EU, USA and Japan alone (4). The estimated global direct cost of osteoporotic fractures is US$ 50 billion per year (3).
Building strong bones and reaching peak bone density (maximum strength and solidness), especially before the age of 30, can be the best defense against developing osteoporosis. Furthermore, a healthy lifestyle can keep bones strong, especially for people over the age of 30. Osteoporosis is more or less preventable for most people. Prevention is very important because, while treatments for osteoporosis are in place, currently no cure exists. Prevention of osteoporosis involves several aspects, including nutrition (see below) and exercise. Loss of muscle strength and mass, especially in the absence of physical activity, can reduce bone strength and stability, increasing the risk of falling and breaking a bone.
Early detection of low bone mass (osteopenia) or osteoporosis is the most important step for prevention and treatment. The only way to accurately test the strength and solidness of the bones is with bone mineral density (BMD) tests. Bone mineral density tests measure the solidness and mass (bone density) of bones in the spine, hip and/or wrist, which are the most common sites of fractures due to osteoporosis.
 Bone loss can lead to
Bone loss can lead to 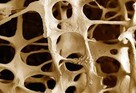 Bone loss
Bone loss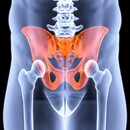 Osteoporosis
Osteoporosis Early prevention
Early prevention Vitamin D and calcium
Vitamin D and calcium Other micronutrients
Other micronutrients